I got published in a philosophy journal.
In 2024, JAMA Pediatrics published “Infant Deaths After Texas’ 2021 Ban on Abortion in Early Pregnancy,” which argued that “abortion restrictions may have negative spillover effects on infant health.”
The paper was filled with questionable and frankly ableist assumptions, and I wanted to respond somewhere beyond SPL’s blog.
I spoke with Nicholas Colgrove about it. He’s a PhD in philosophy and has published extensively on abortion and other topics in bioethics. We decided to co-author a response, and I’m happy to report that our article has been published in The New Bioethics: “Abortion and Infant Mortality: Termination Does Not Prevent Death.”
I was especially proud to contribute substantially to this passage about “the systemic, documented phenomenon of providers pressuring parents to abort in the face of ‘adverse’ prenatal diagnoses.”
A study by Meredith et al. (2024) found that the ‘majority’ of providers exhibited ‘biases’ when discussing the results of prenatal testing with patients. This includes ‘explicit bias’ – such as ‘perpetuating harmful societal stereotypes about people’ with disabilities – and ‘implicit bias,’ which involved delivering diagnoses on the assumption that ‘life with a disability … is bad news’ (Meredith et al. 2024, p. 8). The authors (2024, p. 8) also conclude that providers’ biases in many of these cases caused ‘lasting trauma to parents’ and limited ‘the information and prenatal care they need[ed] at a vulnerable time.’
Relatedly, Farrelly et al. (2012, p. 814) found that ‘when discussing options available if a pregnancy were diagnosed with a disability,’ 86% of genetic counsellors ‘mentioned termination … while fewer mentioned the continuation of pregnancy (37%).’ Medical providers relaying partial information or emphasising some factors over others are subtler ways of pressuring patients toward termination. For example, Ostertag (2022, p. 233) – following Parens and Asch (1999) – observes that ‘the delivery of information about disability and prenatal diagnosis is largely framed to support termination,’ rather than continued pregnancy.
Sometimes providers’ pressure to terminate is overt. Parents of children with Down syndrome (who chose not to terminate) report judgmental, coercive responses from providers, including:
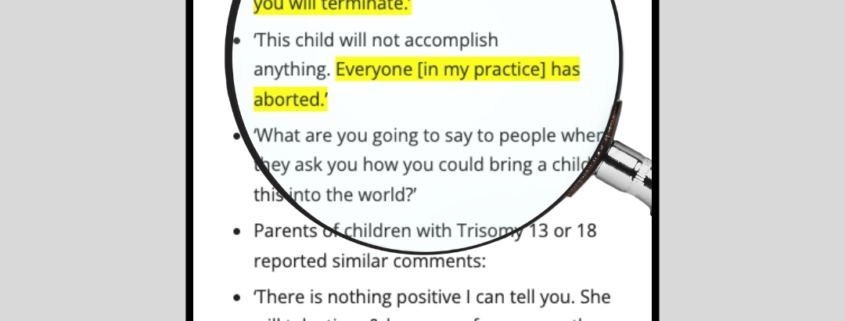
- ‘I’m giving you 5 days to decide which day you will terminate.’
- ‘This child will not accomplish anything. Everyone [in my practice] has aborted.’
- ‘What are you going to say to people when they ask you how you could bring a child like this into the world?’
Parents of children with Trisomy 13 or 18 reported similar comments:
- ‘There is nothing positive I can tell you. She will take time & love away from your other children. She will make your life difficult.’
- ‘There is one simple decision: terminate and get on with your life. It’s a no brainer.’
- ‘Why are you here if you are just waiting for this retarded baby to die?’
So, while Gemmill et al. assume that parents would want to terminate pregnancies with ‘congenital anomalies,’ this overlooks long-standing ableism and paternalism within the medical community.
This research reinforces what we already knew anecdotally. The stories of parents pressured to abort in the face of prenatal diagnoses are legion.
It’s important that the academic record better reflect this ongoing travesty. I’m grateful to Dr. Colgrove for collaborting, and to The New Bioethics for publishing.
If you appreciate this kind of intellectual rigor in pro-life work, please support my efforts here.
Glad to have you in our corner.