Treatment for Ectopic Pregnancy is Not Abortion
[Today’s guest article is by John Bockmann.]
Ectopic pregnancy can be a life-threatening emergency for a pregnant woman. It’s the leading cause of maternal mortality in the first trimester, when most induced abortions occur.
That’s probably why it’s drawn a lot of attention, especially since legal, non-therapeutic abortion is no longer guaranteed everywhere in the United States. There’s a popular myth that ectopic pregnancy is treated by “abortion,” and that abortion bans will, by definition, ban that treatment.
The Fort Worth Star-Telegram, for example, claims that treatment of ectopic pregnancy is abortion. Tweets by Halle Berry and a pastor named Elizabeth warn that if you can’t get an abortion for an ectopic pregnancy, “you die. You. Die.” Even the American College of Obstetricians and Gynecologists (ACOG)’s advocacy statement says that “Abortion bans threaten to impede ectopic pregnancy treatment,” though it doesn’t cite specific bans or make suggestions for clarifying language.
Given abortion’s emotionally-charged implications, misunderstandings become magnified, so it’s crucial to set the record straight right away. Gratefully, this a topic on which the pro-choice and pro-life sides already agree:
According to the CDC, induced abortion–the kind of abortion we’re all talking about–only deals with intrauterine (“inside the uterus”) pregnancy.
Thus, the treatment for ectopic pregnancy—”outside the uterus” pregnancy—is not induced abortion. It is surgical separation of mother and embryo or killing the embryo with methotrexate, described medically as “treatment of ectopic pregnancy.”
Since an ectopic baby cannot (with today’s technology) be carried to delivery, “abortion” doesn’t apply to ectopic pregnancy in the same way it does to most other pregnancies. The baby always dies. We treat ectopic pregnancies to ensure the mother lives.
Consider this tweet from a popular pro-abortion OB/GYN, Jennifer Gunter, M.D.: “We don’t call treatment of ectopic pregnancy [an] abortion, we call it treatment of ectopic pregnancy. We don’t do abortions for ectopic pregnancy, we do medical [or] surgical treatment of ectopic pregnancy.”
Or this from Planned Parenthood’s website: “Treating an ectopic pregnancy isn’t the same thing as getting an abortion.”
The American Association of Pro-Life Obstetricians and Gynecologists agrees, differentiating between “elective abortion” and “treatment of ectopic pregnancy.”
This may seem too fine a point when “treatment of ectopic pregnancy” results in the death of the baby every time, if she’s not already dead. It’s a useful distinction, though, because the term “abortion” can mean three wildly different things: 1) miscarriage, 2) medically required pregnancy termination, or 3) the targeted, unjust killing of an unborn child. It’s easy to conflate these by ignorance or intent, and we ought to welcome any opportunity to clarify the jargon.
As an aside: abortion pills cannot treat ectopic pregnancy, which must be diagnosed with ultrasound and treated by a doctor. They can mask symptoms of ectopic pregnancy, putting women in life-threatening danger. This is a grave concern with the proliferation of mail-order abortion pills.
Moreover: abortion laws make exceptions for the life of the mother, so treatment of ectopic pregnancy would be legal either way. Many laws explicitly preclude ectopic pregnancy from consideration.
I do hate that ectopic pregnancy pits child against mother, and I want to focus our research on preserving both lives. But it’s clear, and experts on both sides agree: treatment of ectopic pregnancy is not abortion. It is treatment of ectopic pregnancy.
More information:
What is abortion?
The United States Centers for Disease Control (CDC) defines induced abortion as “intended to terminate a suspected or known ongoing intrauterine [inside the uterus] pregnancy … that does not result in a live birth.”
What is ectopic pregnancy?
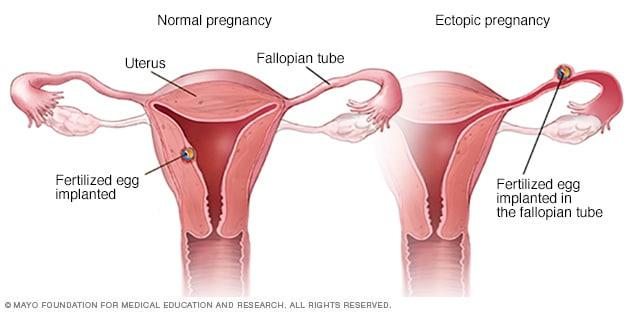
- Ectopic: the embryo has implanted out of place, meaning outside the uterus. Because the vagina opens to the uterus, the uterus opens to the fallopian tubes, and the fallopian tubes open to the abdomen, the list of locations where the embryo could implant is pretty long. Still, only 2% of all pregnancies are ectopic, and more than 90% of these occur in a fallopian tube, which is why they’re sometimes called “tubal pregnancies.”
Risk factors: about half of the women who experience ectopic pregnancy have no identifiable risk factors. But generally, risks include tubal inflammation, deformity, scarring—anything that can make it more difficult for the embryo to move through the fallopian tube to the uterus, including previous ectopic pregnancy, sterilization/tubal surgery, use of IUD, in vitro fertilization, oral contraceptive use, sexually transmitted infections, previous abortion, smoking.
- Diagnosed by transvaginal ultrasound and blood-drawn pregnancy test. If there are symptoms, they’re usually vaginal bleeding and/or abdominal pain, sometimes radiating to a shoulder, around six to eight weeks after last menstrual period.
- Treatment
- Expectant management: also known as “watchful waiting.” This entails patient monitoring and symptomatic treatment. A 1998 study found that about one-in-four ectopic pregnancies resulted in tubal rupture, which can cause life-threatening internal bleeding. Over 50 percent of patients are asymptomatic before tubal rupture, so expectant management is unusual. Even ardent pro-lifers recognize this.
- Medication: methotrexate (“MTX”), an old chemotherapy agent used for cancer and rheumatoid arthritis, psoriasis, lupus, ulcerative colitis, etc. It inhibits folic acid uptake and DNA synthesis, affecting rapidly-dividing cells more than slowly-dividing ones. This includes rapidly-dividing cells of these diseases, human skin, and rapidly-growing trophoblast as well.
- Surgery: removal of the embryo/fetus, usually entailing salpingostomy (incision of the fallopian tube) or salpingectomy (removal of the fallopian tube).
If you appreciate our work and would like to help, one of the most effective ways to do so is to become a monthly donor. You can also give a one time donation here or volunteer with us here.



“There’s a popular myth that ectopic pregnancy is treated by “abortion,” and that abortion bans will, by definition, ban that treatment.
“The Fort Worth Star-Telegram, for example. . .”
There’s no known treatment for elective fear-mongering.